Infrequently Asked Questions
Understanding Blast-Related Brain Injuries
What is a TBI?
- A TBI (Traumatic Brain Injury) is an injury that affects how the brain works. It can be caused by a blow or jolt to the head or an object penetrating the skull. In the military context, it’s often caused by blasts from explosive devices.
- Mild TBI (mTBI): Often called a concussion. May cause temporary confusion, headache, dizziness, or memory issues. These injuries are often overlooked or underestimated but can have lasting effects, especially if repeated.
- Moderate TBI: Involves loss of consciousness for minutes to hours. Cognitive, physical, or emotional impairments may last for weeks or become permanent.
- Severe TBI: Includes prolonged unconsciousness or coma, and can result in long-term or permanent damage to memory, thinking, movement, sensation, or emotional regulation.
- Headache, confusion, dizziness
- Memory loss or trouble concentrating
- Mood swings or emotional instability
- Sleep disturbances
- Sensory changes (e.g., blurred vision, ringing in the ears)
- Seizures (in more severe or chronic cases)
A blast-related Traumatic Brain Injury (bTBI) is a type of TBI caused specifically by exposure to an explosive blast wave, such as from an improvised explosive device (IED), mortar, RPG, or roadside bomb. Unlike traditional TBIs caused by blunt trauma, bTBIs involve unique physiological effects on the brain due to blast overpressure, even when there is no visible wound or direct impact to the head.
Mechanisms of Injury:
- Blunt force trauma: From falls, car accidents, or being struck.
- Blast waves: Common in military combat (e.g., from IEDs); can injure the brain even without a direct blow.
- Penetrating injuries: Bullets or shrapnel piercing the skull and brain.
- Acceleration-deceleration injuries: Where the brain moves violently within the skull (e.g., whiplash or a fall).
Why It Matters (Especially in GWOT Veterans):
In conflicts like Iraq and Afghanistan, TBIs—especially those caused by blasts (bTBIs)—have become the “signature injury”. They often occur without visible wounds, leading to underdiagnosis or misdiagnosis. Yet they can lead to lifelong physical, cognitive, and emotional challenges if untreated.
What is a bTBI?
- A bTBI (blast-related Traumatic Brain Injury) refers specifically to a TBI caused by exposure to explosive blasts, such as IEDs. These are common in modern warfare and often result in invisible injuries not immediately detectable with standard imaging.
How Does a Blast Injure the Brain?
Blast waves from explosions have several phases that can all affect the body:
- Primary blast injury: Caused by the initial pressure wave from the explosion. This wave travels through the body and especially affects air-filled organs (lungs, intestines) and the brain.
- Secondary blast injury: Caused by shrapnel or debris propelled by the blast.
- Tertiary blast injury: Occurs when the individual is thrown by the blast, striking solid objects.
- Quaternary and quinary injuries: Include burns, inhalation of toxic gases, and immune responses.
In a bTBI, the primary blast wave is the most concerning. It can travel through the skull and disrupt the microscopic structure of brain tissue, blood vessels, and neuronal connections without any sign of external trauma.
Why bTBIs Are So Complex and Dangerous:
- Invisible Injury: Soldiers may not realize they’ve been injured. They might not lose consciousness, and medical staff may miss the injury altogether.
- Delayed Symptoms: Symptoms may take days, weeks, or even months to appear.
- Difficult to Diagnose: CT scans and MRIs often do not show abnormalities, especially in mild cases.
- Multiple Exposures: Many service members experience repeated blast exposures, which can worsen long-term outcomes.
Symptoms of bTBI:
- Headaches, fatigue, dizziness
- Memory loss, confusion, slowed thinking
- Emotional changes: anxiety, irritability, depression
- Sensitivity to light and noise
- Sleep disturbances
- Seizures (in some moderate/severe or cumulative cases)
bTBI in the Context of GWOT:
- bTBI became a signature injury in Iraq and Afghanistan due to widespread use of IEDs.
- Troops in combat zones were often exposed to multiple low-level blasts, leading to cumulative brain damage.
- Many were not treated or recognized until after deployment, if at all.
- bTBI is strongly linked to post-traumatic stress disorder (PTSD), chronic pain, and even increased suicide risk.
How many veterans were injured by blast-related injuries during GWOT?
- Over 467,000 service members and veterans have suffered blast-related injuries during the Global War on Terror (GWOT).
What Happens to the Brain during a Blast
Pressure waves from blasts can cause cellular shearing, swelling, and disruption of brain function—often without visible signs on imaging. These effects are primarily due to the rapid overpressure wave generated by the explosion and its interaction with brain tissue.
Key Effects of a Blast on the Brain:
🔄 1. Rapid Pressure Shifts (Overpressure)
💥 2. Cavitation and Tissue Shearing
🧠 3. Disruption of the Blood-Brain Barrier (BBB)
🔥 4. Inflammation and Long-Term Cognitive Symptoms
- Over time, these processes may increase the risk of neurodegenerative diseases, such as chronic traumatic encephalopathy (CTE).
⚠️ Why a bTBI is Especially Dangerous:
- No external injury may be visible—which leads to underdiagnosis.
- Even mild exposure can have cumulative effects, especially with repeated blasts.
- Standard brain scans (CT, MRI) often fail to detect the microscopic damage.
- Many affected veterans experience symptoms that are misattributed to psychological causes (e.g., PTSD), when the root may be physical brain injury.
How has the Goverment Responded to TBI's?
- Blast-related TBI (bTBI) became the signature injury of the GWOT due to the widespread use of IEDs.
A signature injury is a type of injury that becomes emblematic or highly prevalent during a particular conflict.
- Over 50,000 injuries were directly caused by Improvised Explosive Devices (IEDs).
Impact on Casualty Figures
- In both Operation Iraqi Freedom (OIF) and Operation Enduring Freedom (OEF), IEDs accounted for:
- Over 60% of all combat-related injuries
- Majority of severe injuries, including those requiring long-term rehabilitation
- Between 2003 and 2011 in Iraq, IEDs were responsible for nearly two-thirds of all U.S. troop deaths.
- In Afghanistan, the rugged terrain and reliance on foot patrols made troops even more vulnerable to hidden explosives.
- Approximately 54,000 Purple Hearts were awarded throughout the entire GWOT.
- Up to 90% of injuries caused by blasts may have gone unrecognized or undocumented, implying that hundreds of thousands of Purple Hearts may be unawarded.
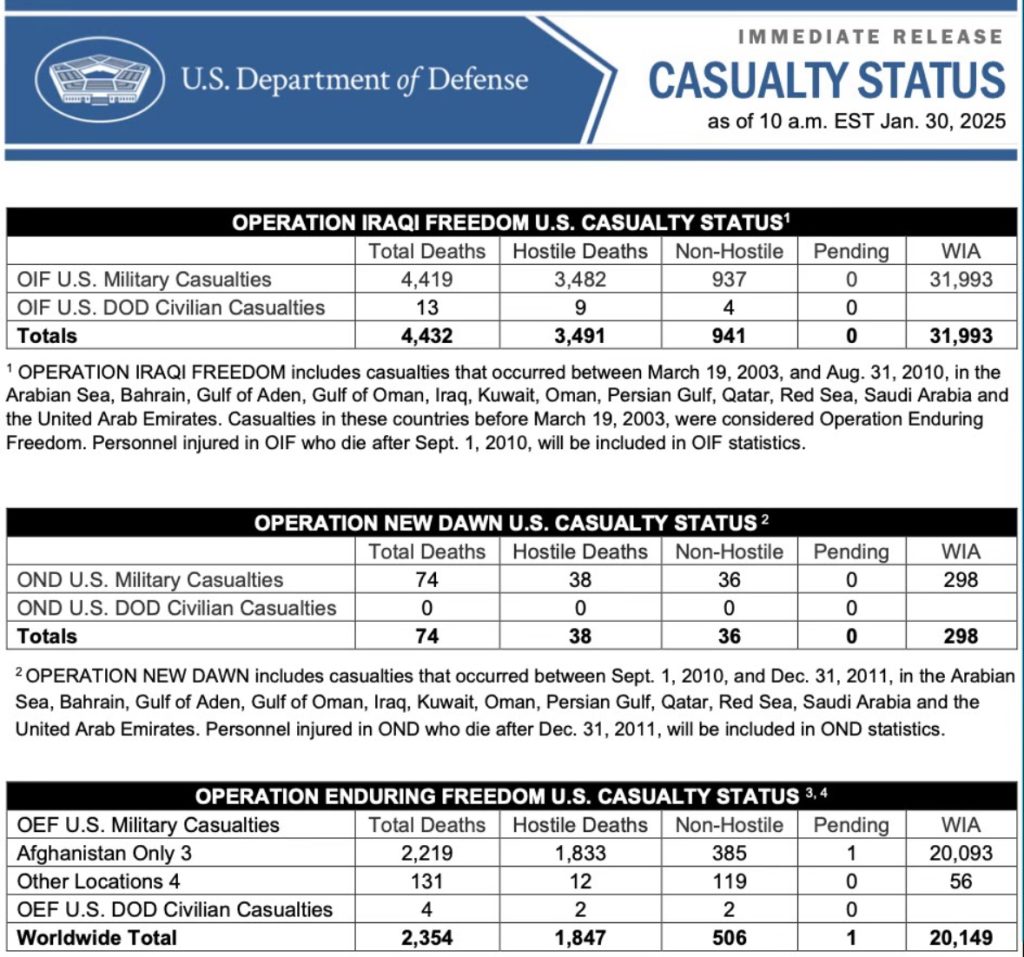
The Human Cost of Blast Injuries
Why is the veteran suicide rate so high?
- Linked to untreated blast injuries, mental health conditions, lack of recognition, and a sense of abandonment.
Why would doctors not give out Purple Hearts even when ordered?
- Some believed only visible injuries counted.
- Fear of setting a precedent for invisible injuries.
- Command influence or image management.
If they were derelict in duty, do service members still qualify for Purple Hearts from IEDs?
Yes. If a service member was injured by enemy action, they qualify — even if a doctor failed to report it at the time.
Why are some brain injuries worse than others, even from the same blast and distance?
Due to differences in:
- Individual brain structure/genetics
- Head orientation or body position
- Prior TBIs (cumulative damage)
- Protective gear, shielding, or terrain
- Secondary projectiles or blast angles
Ignored Injuries and Systemic Injustice
What does a <1% success rate in awarding Purple Hearts for obvious injuries suggest about leadership during GWOT?
Why hasn’t anything been done to help thousands suffering from invisible injuries like seizures?
- There is stigma, limited diagnostics, and institutional resistance to acknowledging such injuries, leading to neglect.
What happens to the brain during an external blast?
- Pressure waves from blasts can cause cellular shearing, swelling, and disruption of brain function—often without visible signs on imaging. These effects are primarily due to the rapid overpressure wave generated by the explosion and its interaction with brain tissue.
Key Effects of a Blast on the Brain:
🔄 1. Rapid Pressure Shifts (Overpressure)
- A blast wave causes a sudden spike in atmospheric pressure that travels through the body.
- The skull and soft tissues compress and rebound rapidly, creating internal pressure changes in the brain.
- This can cause microscopic tearing of neurons and blood vessels, disrupting normal function.
💥 2. Cavitation and Tissue Shearing
- Tiny bubbles (gas or vapor) can form in tissues—called cavitation—and then rapidly collapse.
- This leads to tissue shearing: stretching and tearing of brain structures, particularly at interfaces of different tissue densities (gray vs. white matter).
- These micro-injuries can cause cell death, disconnection of neurons, and long-term neurological effects.
🧠 3. Disruption of the Blood-Brain Barrier (BBB)
- The blood-brain barrier is a protective membrane that regulates what substances can enter the brain from the bloodstream.
- A blast can cause this barrier to break down, allowing toxins, immune cells, and inflammatory molecules to flood into the brain.
- This can lead to neuroinflammation, brain swelling, and further tissue damage.
🔥 4. Inflammation and Long-Term Cognitive Symptoms
- The blast-induced damage often triggers a sustained inflammatory response.
- This chronic inflammation can disrupt neurotransmitters and contribute to symptoms like:
- Memory loss
- Mood disorders (depression, anxiety)
- Sleep disruption
- Impaired concentration and decision-making
- Over time, these processes may increase the risk of neurodegenerative diseases, such as chronic traumatic encephalopathy (CTE).
⚠️ Why It’s Especially Dangerous:
- No external injury may be visible—which leads to underdiagnosis.
- Even mild exposure can have cumulative effects, especially with repeated blasts.
- Standard brain scans (CT, MRI) often fail to detect the microscopic damage.
- Many affected veterans experience symptoms that are misattributed to psychological causes (e.g., PTSD), when the root may be physical brain injury.
Understanding Stem Cell Treatment at Blastology
What Is Stem Cell Treatment?
It involves using undifferentiated cells to repair or replace damaged tissues.
Stem cell treatment (or stem cell therapy) is a form of regenerative medicine that uses stem cells—cells with the unique ability to develop into many different cell types—to repair, replace, or regenerate damaged tissues or organs in the body.
🔬 What Are Stem Cells?
Stem cells are the body’s raw materials—unspecialized cells that can:
- Self-renew (make copies of themselves)
- Differentiate into specialized cells like neurons, muscle cells, or blood cells
There are several types:
- Embryonic stem cells: Can become any cell type (pluripotent)
- Adult stem cells (e.g., from bone marrow or fat): More limited in what they can become
- Induced pluripotent stem cells (iPSCs): Adult cells genetically reprogrammed to behave like embryonic stem cells
⚕️ What Is It Used For?
Stem cell treatment is being researched or used for:
- Blood disorders: Leukemia, lymphoma (bone marrow transplant)
- Orthopedic injuries: Repairing cartilage, ligaments, or bone
- Neurological conditions: Traumatic brain injury (TBI), spinal cord injury, Parkinson’s disease
- Heart disease: Replacing damaged heart tissue
- Autoimmune diseases: Modulating the immune response in MS, lupus, etc.
In the case of TBI or bTBI, experimental treatments aim to:
- Reduce inflammation in the brain
- Regrow damaged neurons
- Restore lost brain function
How Can Stem Cells Help Veterans Suffering from TBIs?
- Stem Cells regenerate damaged brain tissue, reduce inflammation, and restore lost neural connections.
- Stem Cells also help reduce depression, PTSD symptoms, and reduce overall veteran suicide rates.
Why Blastology Does Not Use Donated Cells
- Foreign cells have a potential for immune reaction. This is a risk we cannot take in an already damaged brain.
- There is no way to guarantee ethically sources stem cells if they are donated. Currently, only patients self replicated cells are permitted for use in US treatments.
Effects of Stem Cell Treatment
- Improved motor control
- Restored speech
- Reduced Migraines
- Amplified stamina, reduced fatigue
- Emotional control
- Progressed short term memory
Who is Scuba Steve?
- Scuba Steve is a mythic hero who fought Taliban forces in Afghanistan during 2007-2008. Scuba patrolled rivers and lakes of the Dey Chopan Valley using unconventional warfare, hiding weapons in rivers, drowning his victims.
- Scubas weapon of choice was the water proof AT-4 and hand grenades.
- Dr. Scuba Steve also holds a PH.D in Blastology.
